HOME Cancer
Podcasts

Cancer patient rep has new title: Breast cancer survivor
Podcast: Lynn Roemeling shares her journey from employee to patient at Sanford Health

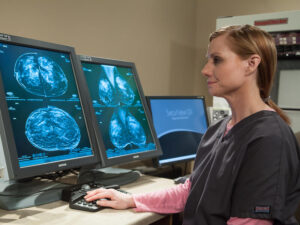
Mammogram callbacks: Should you be worried?
Podcast: Sanford Health radiologist Chris Johansen, MD, eases anxiety about breast cancer imaging

Colon cancer awareness and the importance of screenings
Podcast: Colorectal screenings are vital steps against colon cancer that start at age 45

Importance of getting the HPV vaccine
Podcast: Dr. Brooke Jensen discusses HPV vaccine's role in preventing certain cancers

Blood and bone marrow transplant care at Sanford
Podcast: Providing a second chance by using the patient's own stem cells for treatment

Sanford Health, NCI connect to study, prevent cancer
Podcast: The 'Connect' study will follow participants for 10+ years
Preparing for your first mammogram
Podcast: When scheduling your first mammogram, you may have questions. Dr. Christina Tello-Skjerseth shares what to expect
Food and nutrition tips after cancer diagnosis
Podcast: Keep a balanced approach to help your body work through cancer, chemotherapy

Committing to a cure for cancer
Podcast: Through CAR T-cells, Dr. Carl June has found a way to fight leukemia

Supporting the caregiver beyond cancer diagnosis
Podcast: Reminding all caregivers they are not alone
Recent Stories

Understanding cervical cancer: signs, causes & risk factors
HPV vaccination and routine screenings can help prevent cervical cancer

Perham cancer patient thankful for treatment in hometown
Weekly cancer treatments that used to take 3 hours round trip are now minutes from home

What you need to know about HPV
Learn about human papillomavirus: its causes, symptoms and how to prevent it

Should you get a PSA screening?
Sanford doctor spells out prostate cancer test pros and cons

Lung cancer: Chances, symptoms and prevention
Should you get screened for lung cancer? Yes – if you have certain risk factors

Retired missionary, author graduates to independent living
Cancer survivor moves from nursing home to assisted living to independent apartment

Breast cancer survivor returns to work with cancer patients
For 13 years, she has helped get patients checked into the cancer center

Annual mammogram catches cancer early for Sanford provider
Don’t wait to schedule your yearly mammogram, says Rebecca Roemen, PA-C

Recognizing anxiety and depression in cancer patients
When to add mental health care to your treatment plan, and how caregivers can help

Becker’s names Roger Maris Cancer Center to top 100 list
Health publication honors oncology programs for innovation, discovery, access to care
Cancer
Children's Health
Heart
Orthopedics
Research
Senior Services
Innovations
News
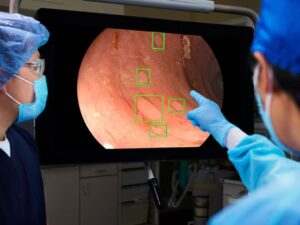
- Sanford Fargo now offers AI-assisted colonoscopies
- Sanford USD Medical Center makes World’s Best Hospitals list
- Sanford earns 3 of Top 100 Critical Access Hospital Awards
- Sanford addresses telehealth’s role in rural communities
- 2 Good Samaritan Society leaders named national Rising Stars
- More in News
Sanford Health Foundation
- Employees Give $416,022 During Month-long Celebration of Gratitude
- Meet Isaac, the 2024 Ambassador for Sanford Children’s in Sioux Falls
- Honoring Norma Peltier: A Legacy of Giving For Good In Fargo
- One Last Wish to Make a Difference
- Owen’s Story: Beating the Odds With Support from Sanford Children’s
- More in Sanford Health Foundation